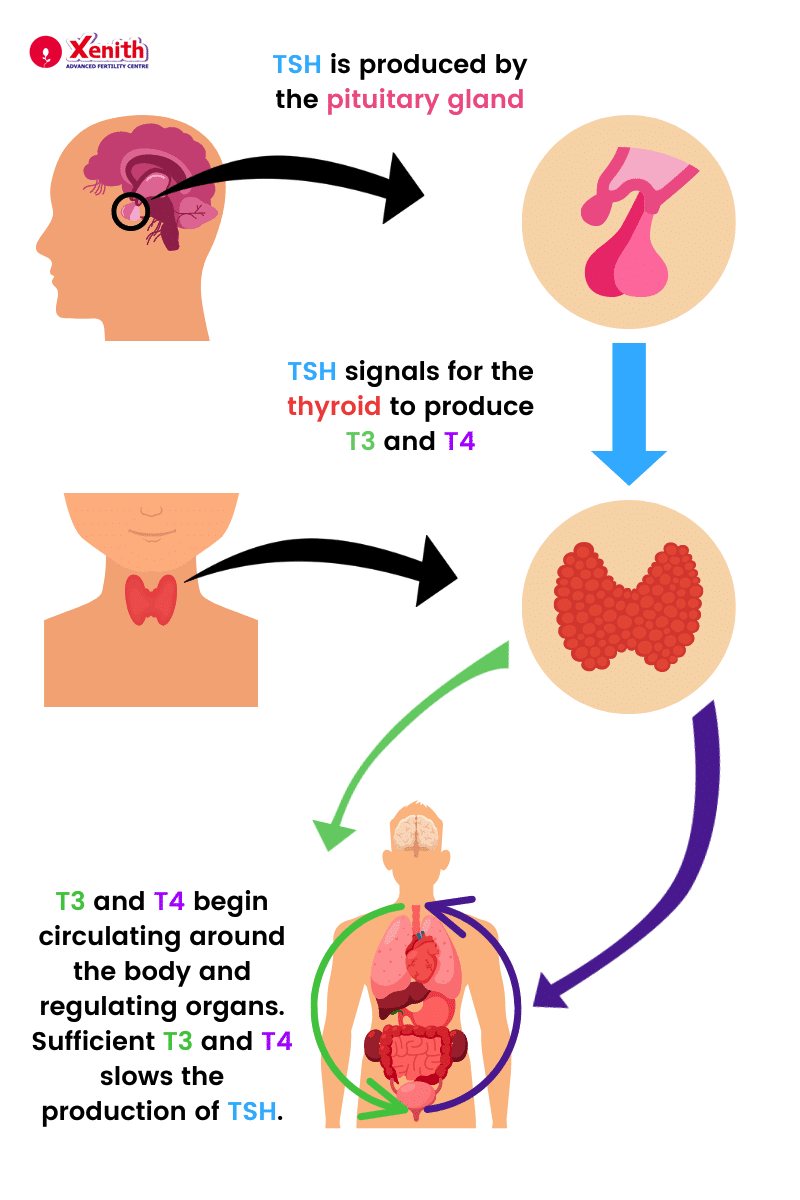
Autoimmune Thyroid Disease and Fertility: Diagnosis, Treatment, and IVF Success Strategies
If you are a woman in Pune trying to conceive and have been told you have a thyroid problem, you are not alone. Hypothyroidism, hyperthyroidism, and autoimmune thyroid diseases like Hashimoto’s are very common among Indian women. Many patients hear…