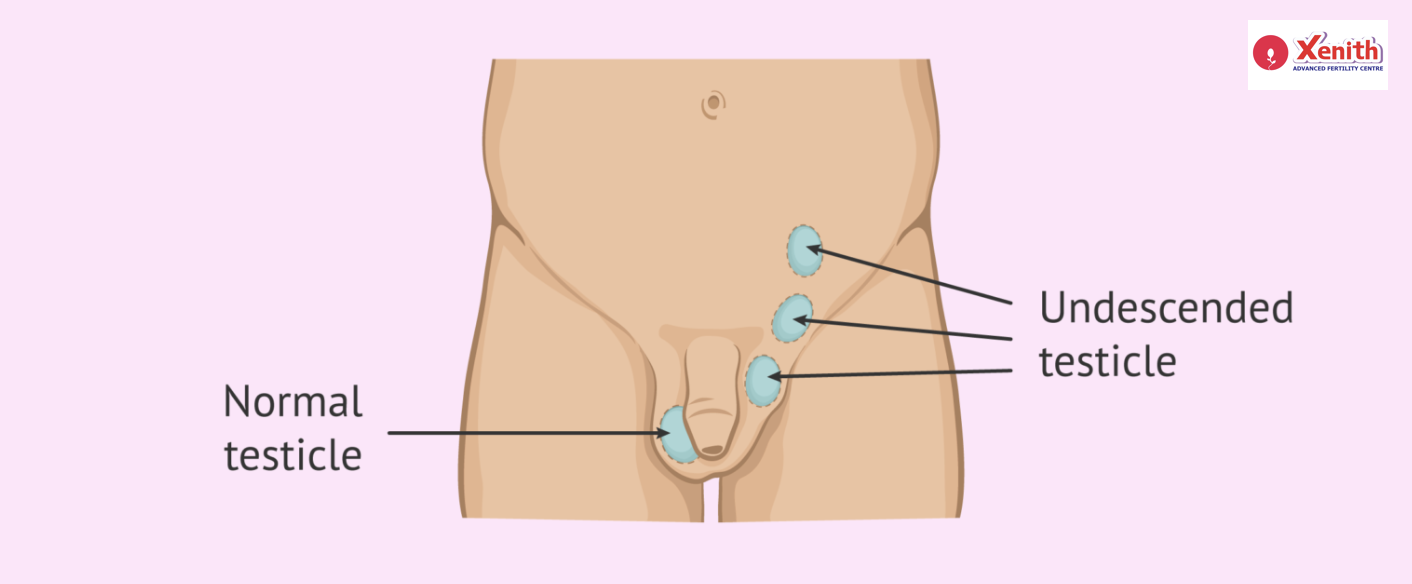
Cryptorchidism (Undescended Testicles) and Future Fertility: What Parents Should Know
As a parent, few things matter more than your child’s long-term health and future well-being. When you hear a medical term like cryptorchidism—especially during infancy or childhood—it can feel overwhelming. You may immediately worry about surgery, long-term consequences, or even…