Asherman’s Syndrome: Symptoms and Severity
For many women trying to conceive, the focus is often on ovulation, egg quality, or sperm health. However, another important factor is the condition of the uterus itself. The uterus is where a pregnancy begins and grows, so its internal environment must be healthy.
Asherman’s Syndrome (AS) is a condition where scar tissue forms inside the uterus. These scars are also called uterine adhesions or intrauterine scarring. When these adhesions develop, they can partially or completely stick the walls of the uterus together. As a result, the uterus may not function normally.

Free Thursday Consultation
Book Your AppointmentIn many women, this condition can lead to menstrual irregularities and infertility. Some patients notice their periods becoming very light or stopping altogether after a surgical procedure. Others may struggle with repeated miscarriages or implantation failure during IVF.
The encouraging news is that Asherman’s Syndrome is treatable. With proper diagnosis and advanced fertility treatment, it is often possible to restore the uterine cavity and improve the chances of pregnancy.
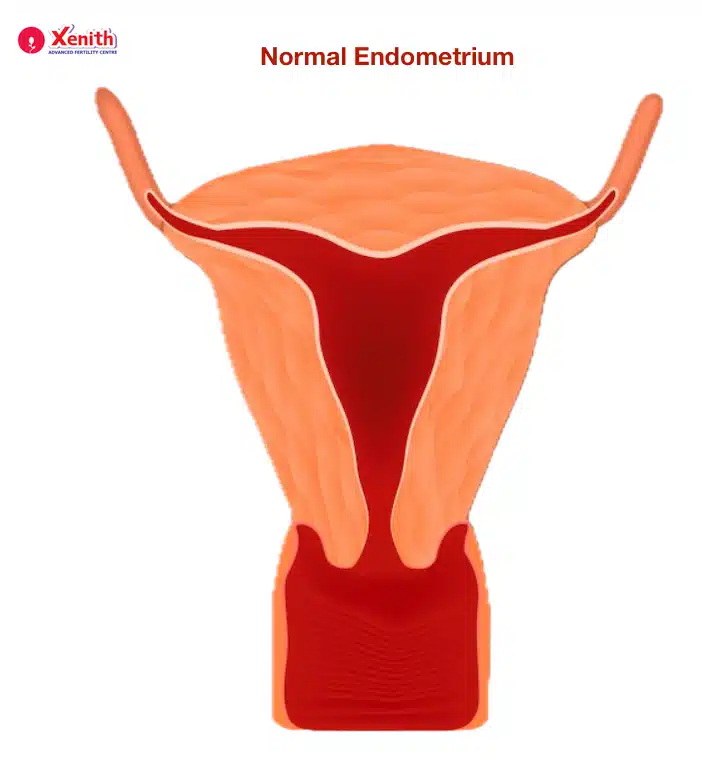
The uterus plays a central role in both menstruation and pregnancy. Inside the uterus is a soft, specialized lining called the endometrium.
In a healthy reproductive cycle:
- The endometrium thickens every month under the influence of hormones.
- This lining prepares itself to receive and nourish an embryo after fertilization.
- If pregnancy does not occur, the lining sheds during menstruation, which we know as a period.
This monthly cycle ensures that the uterus remains a supportive environment for pregnancy.
However, when scar tissue forms inside the uterus, the normal endometrial lining cannot grow properly. This disrupts menstruation and can also make it difficult for an embryo to implant.
The Patient Profile: Who Develops Asherman’s Syndrome?
Asherman’s Syndrome usually develops after a medical procedure or infection that affects the uterus.
Many patients with this condition have a history such as:
- A D&C (Dilatation and Curettage) procedure after a miscarriage.
- Surgical removal of retained placental tissue after delivery.
- A past uterine infection, especially severe endometritis.
- Previous uterine surgeries.
For example, a woman may have normal periods before a miscarriage. After undergoing a D&C procedure, she may notice that her periods become extremely light or even stop completely. Later, when she tries to conceive again, pregnancy does not happen easily.
This change in menstrual pattern can be an early sign of intrauterine scarring.
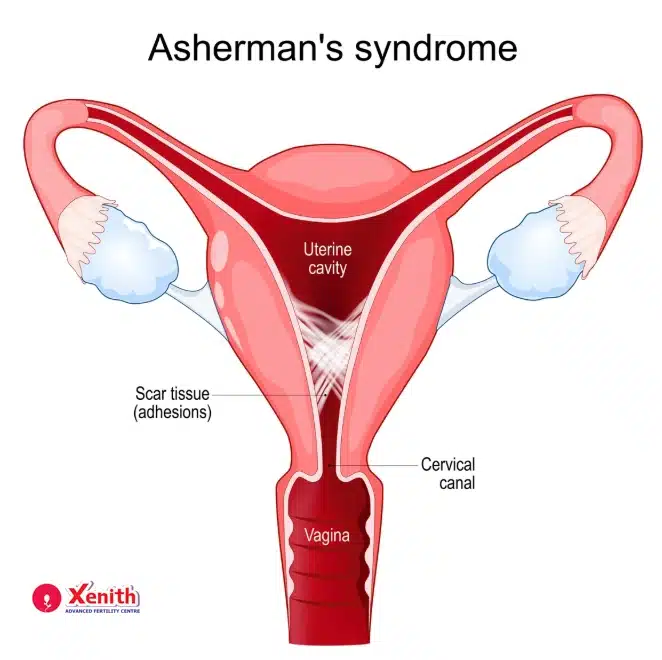
Asherman’s Syndrome: Symptoms and Severity
Not every woman with Asherman’s Syndrome experiences the same symptoms. The severity of the condition depends on how much scar tissue is present inside the uterus.
Some women may have only small adhesions, while others may have large areas of the uterus affected. The more extensive the scarring, the greater the impact on fertility.
Key Symptoms: When to Consult a Specialist
Women should consider consulting a fertility specialist if they notice the following symptoms, especially after a uterine procedure:
- Hypomenorrhea – very light or unusually short menstrual periods.
- Amenorrhea – absence of periods after a D&C or uterine surgery.
- Recurrent miscarriage – repeated pregnancy losses.
- Implantation failure during IVF treatments.
- Pelvic pain in some cases, especially if the cervix becomes partially blocked.
One of the most common patterns seen in clinics is when a patient reports that her periods changed dramatically after a procedure. This change should not be ignored, especially when fertility is a concern.
How Uterine Adhesions Affect Fertility
The main problem with Asherman’s Syndrome is that scar tissue replaces the healthy endometrial lining.
This causes several issues:
- The endometrium cannot grow normally.
- Blood supply to the uterine lining becomes reduced.
- The uterus may lose its natural shape or cavity.
Because of these changes, the uterus becomes a less supportive environment for an embryo. Even if fertilization occurs, the embryo may not be able to implant successfully.
This is why some women experience recurrent implantation failure during IVF. The embryo may be healthy, but the uterus cannot support implantation due to scarring.
Diagnosis and Grading
Diagnosing Asherman’s Syndrome involves examining the structure of the uterine cavity. Unlike hormonal issues, which are detected through blood tests, this condition requires visual assessment of the uterus.
Fertility specialists use imaging techniques and minimally invasive procedures to identify the presence and severity of adhesions.
What Causes Uterine Adhesions?
Several medical situations can lead to uterine scarring. The most common causes include:
- D&C procedures after miscarriage or retained placental tissue.
- Post-partum hemorrhage that requires surgical management.
- Severe uterine infections, such as endometritis.
- Myomectomy (fibroid removal surgery).
- Cesarean section procedures in rare cases.
Among these, repeated or complicated D&C procedures are considered the most common cause of Asherman’s Syndrome.
Diagnosis by a Fertility Specialist
Specialists use a combination of imaging tests and direct visualization to diagnose uterine adhesions.
The most reliable methods include:
Hysteroscopy
This is considered the gold standard for diagnosing Asherman’s Syndrome. A thin camera is inserted through the cervix into the uterus. The doctor can directly see the uterine cavity and identify any adhesions.
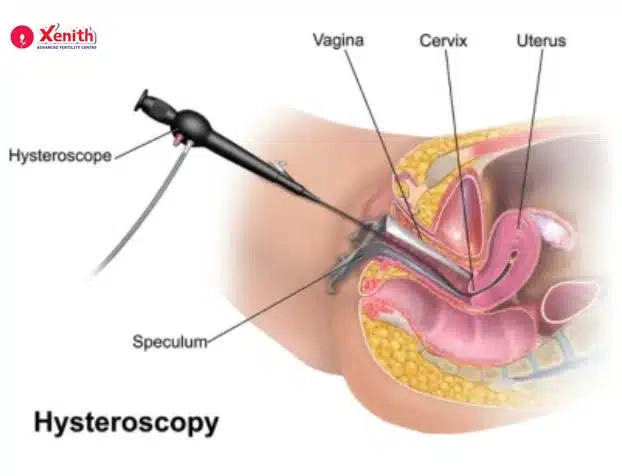
Hysteroscopy also helps classify the condition as:
- Mild
- Moderate
- Severe
This grading is important because it helps determine the treatment plan and prognosis.
Saline Infusion Sonohysterography (SIS)
In this test, saline is gently infused into the uterus during an ultrasound. The fluid helps outline the uterine cavity and may reveal abnormal areas where adhesions are present.
Hysterosalpingogram (HSG)
This is an X-ray test in which contrast dye is injected into the uterus and fallopian tubes. It can suggest the presence of uterine adhesions and is often used as an initial screening test in fertility evaluations.
Treatment—Hysteroscopic Adhesiolysis
Once Asherman’s Syndrome is diagnosed, treatment focuses on restoring the normal uterine cavity.
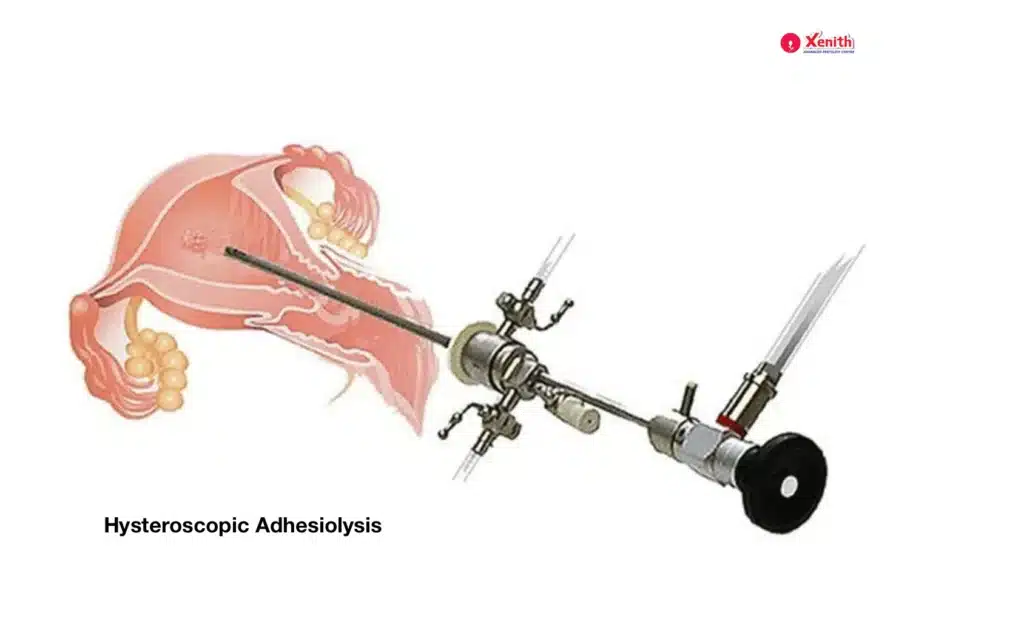
The primary approach is a minimally invasive surgical procedure.
Adhesiolysis: The Surgical Solution
The standard treatment for uterine adhesions is called hysteroscopic adhesiolysis.
During this procedure:
- A hysteroscope is inserted into the uterus.
- Specialized surgical instruments are used to carefully cut and remove the scar tissue.
- The goal is to recreate the normal shape and volume of the uterine cavity.
Because the procedure involves delicate structures, it must be performed by a highly experienced fertility surgeon.
In many cases, restoring the uterine cavity leads to the return of normal menstrual cycles and improved fertility outcomes.
Post-Operative Management to Prevent Recurrence
After surgery, doctors take several steps to help the uterus heal properly and prevent adhesions from forming again.
These may include:
- Estrogen Therapy
Hormonal medication is prescribed to stimulate the growth of a healthy endometrial lining. - Anti-Adhesion Barrier
Doctors may place a temporary device such as a balloon catheter or special gel inside the uterus. This keeps the uterine walls separated while healing takes place. - Antibiotics
Medication may be given to prevent infection during the recovery period.
These measures are important because preventing recurrence is a key part of successful treatment.
FAQs: Common Questions on Asherman’s Syndrome
What is the success rate of the surgery?
The success rate depends on how severe the adhesions are. Mild to moderate cases usually have a very high success rate for restoring menstruation and improving fertility. Severe cases may require more complex treatment, but they can still be managed successfully.
How long after surgery can I try to conceive?
Most doctors recommend waiting for one to three menstrual cycles after surgery. This allows the uterine lining to heal and regrow properly, often supported by hormonal therapy.
Will Asherman’s Syndrome cause problems in a future pregnancy?
After successful treatment, many women carry their pregnancies to term. However, there may be a slightly higher risk of complications such as placenta accreta or preterm delivery. Regular monitoring by a specialist is therefore important.
Can Asherman’s Syndrome recur after treatment?
Yes, recurrence can occur, especially in severe cases. This is why post-operative treatment and follow-up hysteroscopy are sometimes recommended.
Conclusion: A Clear Path to Uterine Health
Asherman’s Syndrome can be a distressing diagnosis, particularly for women trying to conceive. However, it is important to remember that uterine adhesions are treatable, and many patients go on to achieve successful pregnancies after proper treatment. Early diagnosis, skilled surgical care, and careful post-operative management play a crucial role in restoring uterine health and improving fertility outcomes.
If you have noticed a sudden change in your menstrual flow after a D&C procedure or are facing unexplained implantation failure during fertility treatment, it may be time for further evaluation. Schedule a confidential consultation with our fertility specialists at Xenith IVF, Pune today to discuss your personalized Asherman’s Syndrome treatment plan and take the next step toward a healthy pregnancy.